Update time:2026-04-11Visits:2679
In a significant medical breakthrough, a team from Shanghai Ninth People's Hospital, affiliated with Shanghai Jiao Tong University School of Medicine, has diagnosed an exceptionally rare hereditary bone disease with an estimated incidence of just one in a million.
The case, involving a young female patient, was recently published online in Orbit, a leading international journal for orbital diseases.
The patient initially presented at the hospital's Ophthalmology Department with protruding eyes and deteriorating vision. Her symptoms were not isolated to her eyes; she also reported a 15-year history of chronic limb bone pain and progressive hearing loss, having previously been diagnosed with thyroid and gonadal deficiencies at another institution.
A prompt multidisciplinary consultation was convened, bringing together experts from Endocrinology, Molecular Diagnostics, Orthopedics, Imaging, and Otorhinolaryngology. The collective investigation led to a definitive diagnosis: Camurati-Engelmann disease, also known as Progressive Diaphyseal Dysplasia.
From Ocular Symptoms to Systemic Diagnosis
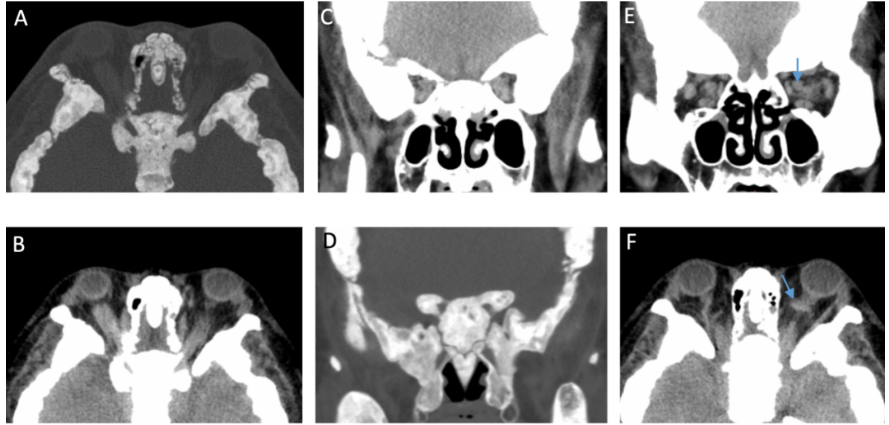
Ophthalmic examinations revealed mild visual field defects and thinning of the retinal nerve fibre layer. Crucially, orbital CT scans showed the root cause: diffusely thickened orbital bone walls, severe narrowing at the orbital apex, and constricted optic canals. These structural changes (indicated by blue arrows in the accompanying image) were compressing the optic nerves. Additionally, dilated superior ophthalmic veins suggested impaired blood flow, likely increasing orbital pressure and further compromising optic nerve function.
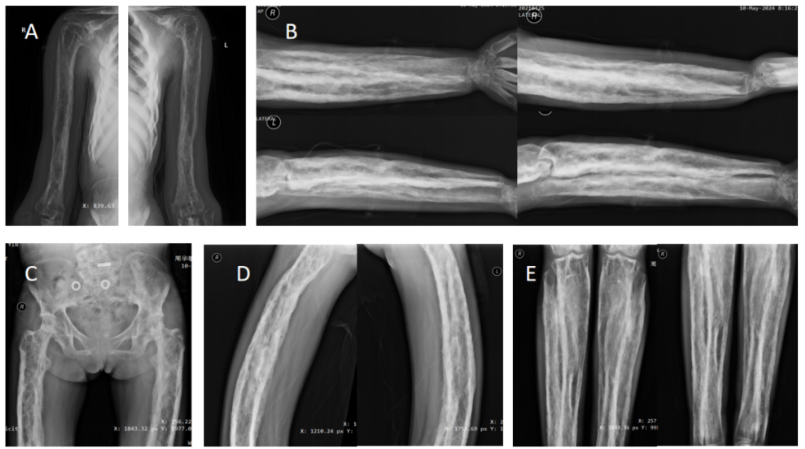
The investigation expanded with full-body X-rays, which confirmed the disease's systemic nature. The images revealed symmetrical cortical thickening and bone enlargement in the shafts of multiple long bones, demonstrating that the condition affected the patient's entire skeleton.
A Clear Genetic Link
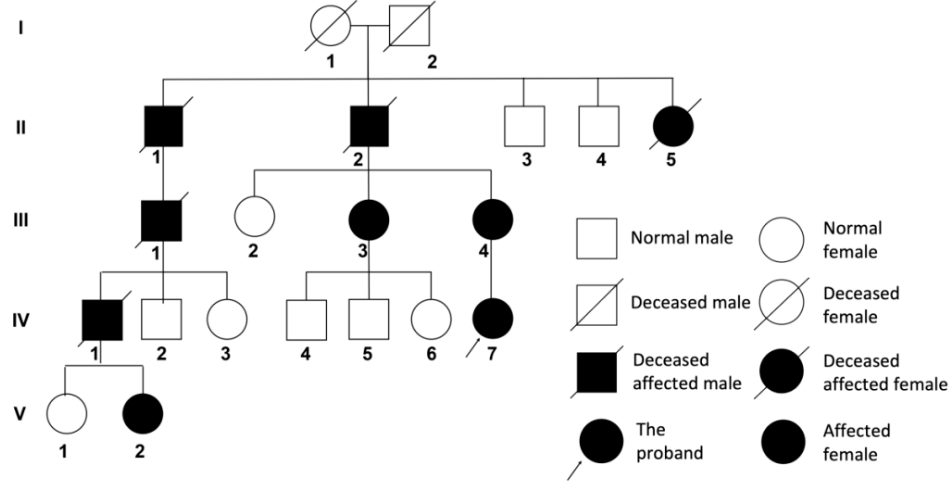
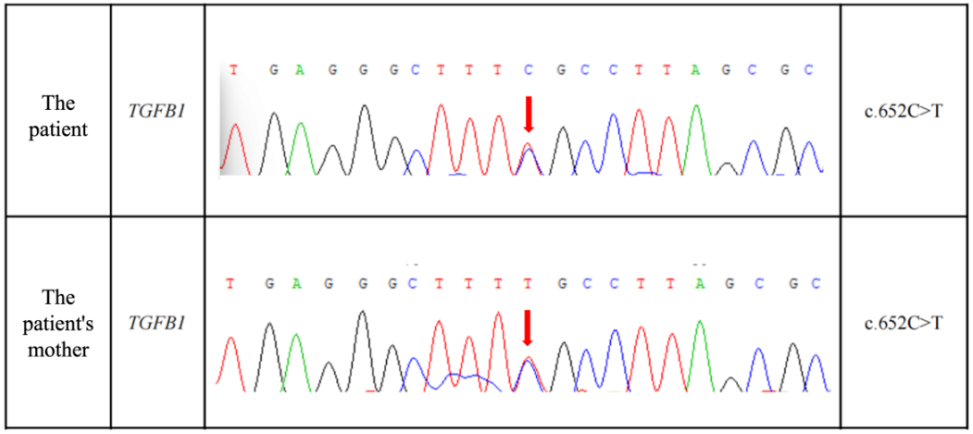
A review of the patient's family history revealed a striking pattern: a total of nine relatives, including her mother, exhibited similar symptoms, indicating a strong hereditary component. Subsequent genetic testing identified a mutation in the TGFB1 gene in both the patient and her mother, confirming the genetic basis of this rare disorder.
This gene encodes transforming growth factor beta 1 (TGF-β1), a key regulator of bone remodelling. Mutations can disrupt the balance between bone formation and resorption, leading to the characteristic thickening of the long bone shafts. Based on the patient’s clinical presentation, alongside haematological, imaging, and genetic evidence, a final diagnosis of Camurati-Engelmann disease was confirmed.
Following a multidisciplinary review, and given the patient’s currently stable vision, treatment prioritised systemic management of the underlying bone metabolism and endocrine abnormalities, with close monitoring of visual function. Should follow-up reveal progressive vision loss or worsening optic nerve damage, surgical interventions such as orbital or optic nerve decompression may be considered to relieve pressure on the nerve.
Notably, the patient’s mother experienced significant symptom relief during and after pregnancy. This phenomenon has been documented in previous case reports, suggesting a potential link to hormonal fluctuations or altered immune regulation. The exact mechanism, however, requires further investigation.
Camurati-Engelmann disease is a rare autosomal dominant genetic disorder, primarily caused by mutations in the TGFB1 gene, with an estimated incidence of 1 in 1 million. It is characterised by symmetrical cortical thickening of the long bones and dysregulated bone remodelling. Typical symptoms include bone pain in the limbs, muscle weakness, and gait abnormalities, which may be accompanied by systemic effects such as endocrine dysfunction. As the disease progresses, it can involve the skull and skull base, potentially leading to headaches, hearing loss, and visual impairment. Given its highly variable presentation, the condition is often misdiagnosed or overlooked. A clear diagnosis and subsequent management typically require a multidisciplinary approach.
The study’s co-corresponding authors are Professor Zhou Huifang of the Department of Ophthalmology and Professor Qiao Jie of the Department of Endocrinology at Shanghai Ninth People’s Hospital, Shanghai Jiao Tong University School of Medicine. The first author is doctoral candidate Lei Chaoyu from the Department of Ophthalmology. Associate Researcher Zhao Shuangxia from the Department of Molecular Diagnostics and Deputy Chief Physician Li Yinwei from the Department of Ophthalmology also contributed jointly to the diagnosis, treatment, and research guidance for this case.
References:
[1] Lei C, He Z, Liang Y, et al. Camurati-Engelmann disease with bilateral proptosis and optic neuropathy: a case report and literature review. Orbit. Published online April 8, 2026. doi:10.1080/01676830.2026.2650802
[2] De Vits A, Keymeulen B, Bossuyt A, Somers G, Verbruggen LA. Progressive diaphyseal dysplasia (Camurati-Engelmann's disease). Improvement of clinical signs and of bone scintigraphy during pregnancy. Clin Nucl Med. 1994;19(2):104-7.
Groundbreaking Diagnosis: Shanghai Medical Team Identifies Ultra-Rare Bone Disorder
Foreign travelers can get service from Shanghai’s community hospital from now on
Shanghai Team Performs First ABO-Incompatible Heart Transplant on Infant
Shanghai Medical Pilot Realizes “Walking Dream” for Bulgarian Girl with Cerebral Palsy
A Shanghai Doctor Uses Ultrasound to “Wake Up” Mother's Alzheimer's
Shanghai Medical Trio Stages High-Altitude Rescue on Flight from Xinjiang
Shanghai Children’s Hospital Uses Remote MDT to Diagnose Rare CIPA
Groundbreaking Diagnosis: Shanghai Medical Team Identifies Ultra-Rare Bone Disorder
Foreign travelers can get service from Shanghai’s community hospital from now on
Shanghai Team Performs First ABO-Incompatible Heart Transplant on Infant

For 54-year-old Malaysian Chinese businessman Mr. Chan, the last three months had been profoundly unsettling. His own hands no longer felt like his own. Simple, everyday acts—fastening a shirt button, holding chopsticks, gripping a pen—had become monumental challenges.

An overseas Chinese was treated from Shanghai Changhai Hospital with successful removal of a pancreatic tumor.

Shanghai Medical Pilot Realizes “Walking Dream” for Bulgarian Girl with Cerebral Palsy

A Shanghai Doctor Uses Ultrasound to “Wake Up” Mother's Alzheimer's

Shanghai Medical Trio Stages High-Altitude Rescue on Flight from Xinjiang

Shanghai Children’s Hospital Uses Remote MDT to Diagnose Rare CIPA

A Seven-Year Lifeline: The Warm Sun of Ovarian Cancer Care